
by Me | Sep 13, 2018 | Diabetes, Pre-Surgery
I was first diagnosed with Type II Diabetes several years ago… and since then have been on a cocktail of different medications (and more recently injections) to get my blood sugar under control.
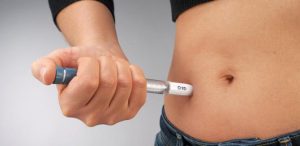 Initially this was a single daily tablets, but over the years has expanded (as the Diabetes “took hold”) to include Insulin injections and also high blood pressure medication.
Initially this was a single daily tablets, but over the years has expanded (as the Diabetes “took hold”) to include Insulin injections and also high blood pressure medication.
just a month ago, I was on 4 different tablets (taken at morning and night) and 7 daily injections of three different Insulin medications (3 in the morning and evening and 1 midday). I was also doing regular (3 or 4 times a day) Blood Prick tests to monitor my blood glucose levels. With all these medications I finally had my blood sugar “under control” but it was still too high… and was only going to get worse with time if I didn’t change something.
I thought I was already eating “pretty well”, but 9 weeks ago, I lost my sense of taste… and as a result… lost interest in food… and also appetite. As a consequence I significantly cut down on what I was eating, and “accidentally” lost 10Kg in 9 weeks.
 My blood sugar levels plummeted, and I found I had to reduce my Diabetes meds and actually make myself eat more than I really felt like eating – just to get my blood sugar above 4 (I am not allowed to drive with a blood sugar less than 5). In the last week I have also started my pre-surgery OptiFAST VLCD Meal Replacement Diet, so my blood sugar continued down and now – 1 week BEFORE my weight loss surgery, I have reduced my Diabetes AND Blood Sugar medications to 2 tablets and 1 injection each evening… and my blood glucose readings haven’t been this good in years.
My blood sugar levels plummeted, and I found I had to reduce my Diabetes meds and actually make myself eat more than I really felt like eating – just to get my blood sugar above 4 (I am not allowed to drive with a blood sugar less than 5). In the last week I have also started my pre-surgery OptiFAST VLCD Meal Replacement Diet, so my blood sugar continued down and now – 1 week BEFORE my weight loss surgery, I have reduced my Diabetes AND Blood Sugar medications to 2 tablets and 1 injection each evening… and my blood glucose readings haven’t been this good in years.
Following surgery I expect to very quickly stop all diabetes/blood pressure medication all together 🙂
I was actually quite shocked over how much difference a very well controlled diet (in my case encouraged by loss of taste) had on my weight and diabetes… I had to start wondering if weight loss surgery is actually necessary, but I am positive that even though I have had great, fast term results, I wouldn’t be able to maintain it, and once my taste returned (it seems to be improving now) I would very quickly slip back into bad habits and my weight/diabetes issues would return.
This is very much supported by research on the long term benefits of weight loss, major studies such as the Swedish Obesity Study and the US Veterans Study show very strong long term benefits of Bariatric Surgery when compared with “traditional” weight loss strategies (diet, exercise, counselling)

by Me | Sep 12, 2018 | Pre-Surgery
Having a gastric bypass can be a life-changing event. This type of surgery is permanent and irreversible so it is good to be fully prepared for surgery both physically and mentally. Ensuring you are fully prepared and ready for the life changes that are about to occur can make recovery and healing much easier, and can also drastically help with the transition into your new lifestyle and eating habits.
My Gastric Bypass Surgery is scheduled in 8 days, and I have done some research into what to expect and how best to prepare for it. I have collated below some tips and suggestions on preparing for gastric Bypass Surgery that I have gleaned from the web… and after the surgery, I may revist this topic to see how well they actually helped to prepare me for the procedure :
1. Pack loose and comfortable clothing for the hospital. It could be difficult to move and bend your body after the surgery so make sure you have clothes that are easy to get into and will not iritate things such as stitches or staples that you may have in your abdomen. Also, Make sure there are extra clothes for your home as well. This means ensuring that your wardrobe is as comfortable for home as it was in the hospital. This can also mean purchasing proper, loose-fitting business clothes if you are planning on returning to work within a short period.
2. Ensure you have shoes that can easily slip on. Slip on shoes will be much easier than having to bend down and have to Velcro or tie shoes.
3. Try to have some “transition” clothing, shoes, etc. These items are usually old clothing that you can no longer fit into but will be perfect as you lose weight. You will start to lose weight dramatically and it is more cost effective to have some older clothing ready than buying new clothes. If you do need to buy new clothes then try charity stores for cheaper alternatives. Only start to buy new clothes once you have stopped losing weight at such a dramatic rate.
4. Purchase multivitamins. It is difficult to get nutrition directly after surgery and multivitamins help immensely. Your dietician will be able to tell you which vitamins you will require to meet your specific needs.
Purchase multivitamins. It is difficult to get nutrition directly after surgery and multivitamins help immensely. Your dietician will be able to tell you which vitamins you will require to meet your specific needs.
5. Have over-the-counter pain medication on hand. After the prescribed pain medication has run out it is prudent to have regular strength medication, such as Tylenol avaiable if necessary.
6.  Stop smoking. Smoking can lead to post-op complications and surgeons may refuse to operate if you still have nicotine in your system. You will normally need to stop smoking 2-4 weeks before surgery.
Stop smoking. Smoking can lead to post-op complications and surgeons may refuse to operate if you still have nicotine in your system. You will normally need to stop smoking 2-4 weeks before surgery.
7. Have someone ready to help you out around the house for the first week or two. You may need someone for physical support and/or to do things around the house such as light cleaning, laundry, etc.
8. Make a list of things you will need for the first few weeks. This will include clear liquids, clear soups, small food containers that are perfect for your new, smaller portions, and protein powder. Make some post-op friendly meals and freeze them into small portions. Remember that they must be high in protein and nutritional value but very low in fat and sugar.
9. Get proper nutrition before surgery. Ensure your body is ready for the surgery and the recovery phase — Eat a proper and varied diet will lots of protein and vegetables. This will help get your body in the best possible shape before having gastric bypass surgery.
10. Read up on the surgery. Make sure you are well educated on your procedure and know what to expect. Talk to others who have already had a gastric bypass and join a support group. Online support groups, such as RealSelf, can provide support, expert knowledge and anonymity.

by Me | Sep 7, 2018 | Pre-Surgery, Weight Loss Surgery Research
A Study initiated by the US Department of Veteran Affairs (
JAMA Surg. 2016 Nov 1; 151(11): 1046–1055.) was undertaken to examine the durability of weight loss for various bariatric procedures as compared with nonsurgical techniques.
 The objective of this study was to examine 10-year weight change in a large, multisite, clinical cohort of subjects who underwent Roux-en-Y gastric bypass (RYGB) compared with nonsurgical matches and the 4-year weight change in veterans who underwent RYGB, adjustable gastric banding (AGB), or sleeve gastrectomy (SG).
The objective of this study was to examine 10-year weight change in a large, multisite, clinical cohort of subjects who underwent Roux-en-Y gastric bypass (RYGB) compared with nonsurgical matches and the 4-year weight change in veterans who underwent RYGB, adjustable gastric banding (AGB), or sleeve gastrectomy (SG).
Differences in weight change up to 10 years after surgery were examined for 1787 subjects who underwent RYGB from January 1, 2000, and 5305 nonsurgical matches. Differences in weight change up to 4 years was also compared among subjects undergoing RYGB (n = 1785), SG (n = 379), and AGB (n = 246). Data analysis was performed from September 9, 2014, to February 12, 2016.
RESULTS
The 1787 patients undergoing RYGB had a mean (SD) age of 52.1 (8.5) years and 5305 nonsurgical matches had a mean (SD) age of 52.2 (8.4) years. Patients undergoing RYGB and nonsurgical matches had a mean body mass index of 47.7 and 47.1, respectively, and were predominantly male (1306 [73.1%] and 3911 [73.7%], respectively).
Patients undergoing RYGB lost 21% more of their baseline weight at 10 years than nonsurgical matches. A total of 405 of 564 patients undergoing RYGB (71.8%) had more than 20% estimated weight loss, and 224 of 564 (39.7%) had more than 30% estimated weight loss at 10 years compared with 134 of 1247 (10.8%) and 48 of 1247 (3.9%), respectively, of nonsurgical matches.Only 19 of 564 patients undergoing RYGB (3.4%) regained weight back to within an estimated 5% of their baseline weight by 10 years.
At 4 years, patients undergoing RYGB lost of their baseline weight, patients undergoing AGB lost 10.6%, and patients undergoing SG lost 17.8%. Patients undergoing RYGB lost 16.9% more of their baseline weight than patients undergoing AGB and 9.7% more than patients undergoing SG.
CONCLUSIONS AND RELEVANCE
Patients receiving bariatric surgery lost substantially more weight than nonsurgical matches and sustained most of this weight loss in the long term. Roux-en-Y gastric bypass induced significantly greater weight loss than SG or AGB at 4 years.

by Me | Sep 6, 2018 | Pre-Surgery, Weight Loss Surgery Research
Weight loss surgery can make a big difference for people with type 2 diabetes. For many people, blood sugar levels get back to normal after surgery (and for Gastric Bypass surgery, this can place before there is even any significant loss in weight). This could mean you need less medication or none at all.

Research shows improvements in type 2 diabetes after weight loss surgery. One long-term study tracking 400 people with type 2 diabetes found that six years after bariatric surgery, 62% showed no signs of diabetes. They also had better blood pressure, cholesterol, and triglyceride levels. In comparison, only 6% to 8% of people who took medicine, but didn’t have surgery, showed similar results.

by Me | Sep 6, 2018 | Food & Diet, Pre-Surgery
Okay… so today I start my 2 weeks pre-surgery Meal Replacement Diet… which essentially involves replacing all meals with OptiFAST Shakes/Soups/Bars with a few fruit and veges in-between – and lots of water.
I’ve been out shopping (spent $150 on OptiFAST) and the photo above shows pretty much everything I will be eating over the next 2 weeks.
- OptiFAST Chocolate/Caramel Shakes
- OptiFAST Berry Crunch Bars (No Chocolate available at the moment)
- OptiFAST Chicken/Vegetable Soups
- Some Veges – I prefer Celery, Carrots and Tomatoes (yeah I know they are really fruit)
- Some Fruit – Berries and Apples – (Not in Photo)
- Plenty of water (I can have carbonated water Before Surgery, but NOT After)… I will have Lemon Juice in it to make it more “interesting”… and I am not really supposed to have the Flavoured Mineral water but that is my secret (not so secret anymore) treat
- Tea (I don’t drink Coffee) without sugar (but I can have skim milk) – I have got a few different varieties of herbal teas to make life a little bit more interesting too.

by Me | Sep 5, 2018 | Food & Diet, Pre-Surgery
Today is the last day that I will eat “real” food for probably 2 months…. and will most likely be a turning point for a change in my food habits for the rest of my life.

Tomorrow I start 2 weeks a pre-surgery “meal replacement” diet, then after surgery I go on liquids for 2-3 weeks – followed by 2-3 weeks of “mush”… and then once I can eat solids again… the size of meals will be significantly restricted… for the rest of my life.
Despite my weight, I don’t consider my food habits particularly bad… I only occasionally had take-away… ate plenty of fruit and veges… drank plenty of water… but clearly the quantity/serving size of my meals was an issue…. That is all about to change … dramatically.

 Initially this was a single daily tablets, but over the years has expanded (as the Diabetes “took hold”) to include Insulin injections and also high blood pressure medication.
Initially this was a single daily tablets, but over the years has expanded (as the Diabetes “took hold”) to include Insulin injections and also high blood pressure medication. My blood sugar levels plummeted, and I found I had to reduce my Diabetes meds and actually make myself eat more than I really felt like eating – just to get my blood sugar above 4 (I am not allowed to drive with a blood sugar less than 5). In the last week I have also started my pre-surgery OptiFAST VLCD Meal Replacement Diet, so my blood sugar continued down and now – 1 week BEFORE my weight loss surgery, I have reduced my Diabetes AND Blood Sugar medications to 2 tablets and 1 injection each evening… and my blood glucose readings haven’t been this good in years.
My blood sugar levels plummeted, and I found I had to reduce my Diabetes meds and actually make myself eat more than I really felt like eating – just to get my blood sugar above 4 (I am not allowed to drive with a blood sugar less than 5). In the last week I have also started my pre-surgery OptiFAST VLCD Meal Replacement Diet, so my blood sugar continued down and now – 1 week BEFORE my weight loss surgery, I have reduced my Diabetes AND Blood Sugar medications to 2 tablets and 1 injection each evening… and my blood glucose readings haven’t been this good in years.


 Stop smoking. Smoking can lead to post-op complications and surgeons may refuse to operate if you still have nicotine in your system. You will normally need to stop smoking 2-4 weeks before surgery.
Stop smoking. Smoking can lead to post-op complications and surgeons may refuse to operate if you still have nicotine in your system. You will normally need to stop smoking 2-4 weeks before surgery.
 The objective of this study was to examine 10-year weight change in a large, multisite, clinical cohort of subjects who underwent
The objective of this study was to examine 10-year weight change in a large, multisite, clinical cohort of subjects who underwent 



